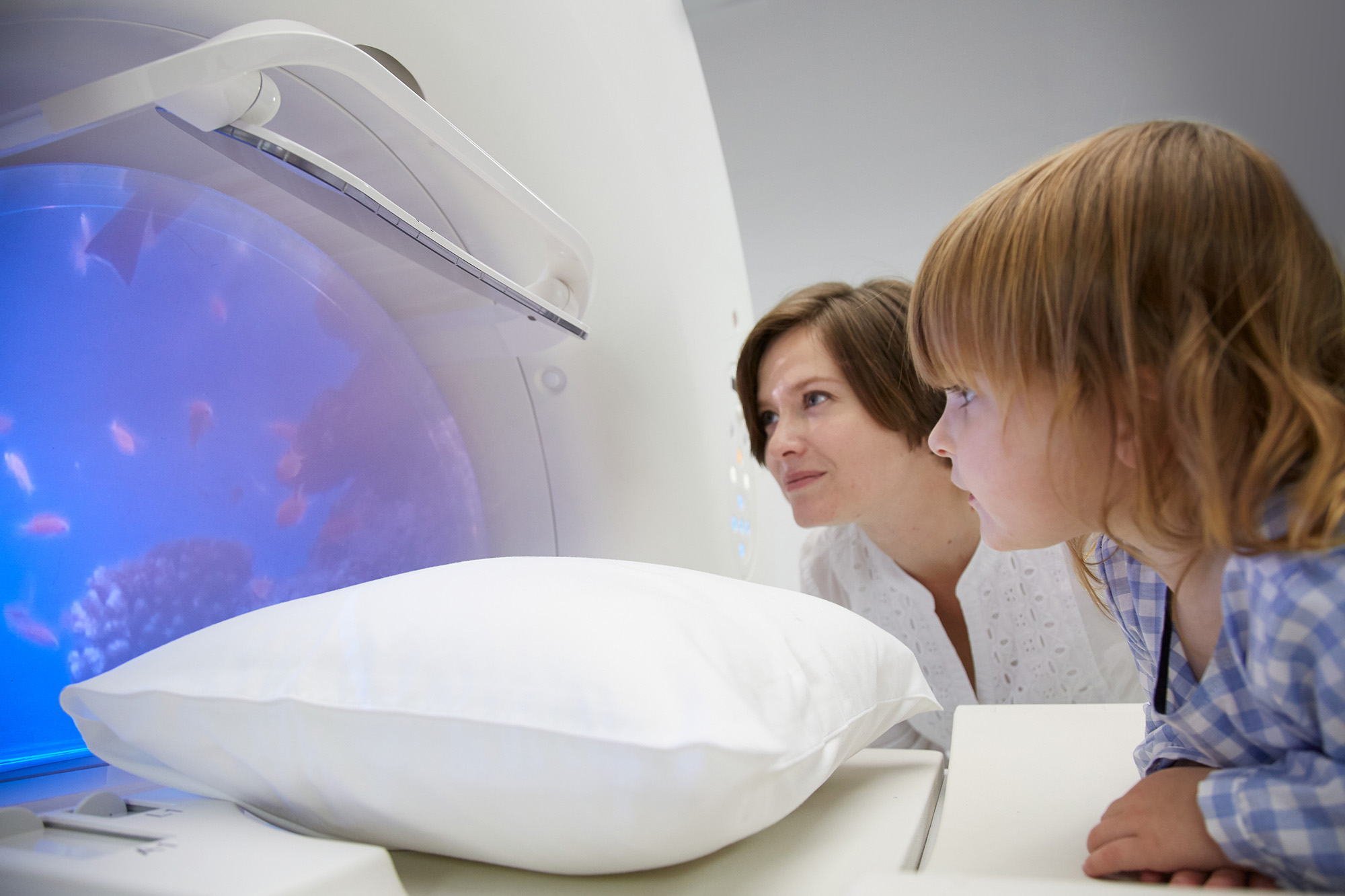
Canon Learning Center
Customized Performance Learning. A daily, long-term commitment.
Evolution of Image Processing: Past, Present & Beyond
Join us for a complimentary, accredited webinar and receive 1 CE credit.
In this webinar we will be discussing: the history of image processing, film screen processing, the evolution to digital processing (which includes both computed and digital), how to assess images and image quality, processing the pros and cons between each generation, the future technologies being developed, and Canon Medical System’s digital radiographic solutions.
Honoring Women in Medicine
Thank you for joining Canon Medical to honor Women in Medicine. Participants can complete the CME survey (if applicable), and CE certificates are available to access.
Webinar - New Advances in CT Technology for Coronary Plaque Assessment
Thank you to those that joined Dr. Dinesh Kalra for the live webinar titled: “New Advances in CT Technology for Coronary Plaque Assessment”.
If you missed the webinar there is a complimentary replay available now. This webinar provides 1 AMA/PRA Category 1 CME credit, and 1 CE credit.
Diagnostic Imaging Interviews Canon Medical's Director of Education Operations
Canon Medical is celebrating Digital Learning Day by offering complimentary continuing education courses. These courses will be available to access online at no charge on Thursday, February 23, 2023

Canon Medical On Demand
Canon Medical On Demand helps you keep pace with the clinical, technical, and practice-related developments in medical imaging through live, accredited, complimentary educational webinars.
Disinfection Guide Library
Canon Medical is making every effort to provide a safe and secure diagnostic environment for both patients and healthcare professionals. To help prevent the spread of infectious diseases at health facilities, we have created a library of disinfectant documentation for our customers.
Service Training
Canon Medical offers up-to-date clinical engineering training programs, developed by engineers for engineers. Our Service Training Team will work with you to customize training that meets your needs.
Featured Courses
Imaging Techniques in Interventional Radiology
In this course, we will discuss select imaging techniques on Canon Medical’s Alphenix vascular system and their clinical applications during interventional radiologic procedures. These angiographic imaging strategies can contribute to advanced system utilization and treatment by clinicians and technologists alike.
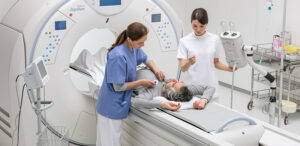
CT Cardiac Best Practices
Join us as we utilize clinical scenarios to illustrate CT cardiac imaging workflows. This course aims to familiarize the technologist with best practice in cardiac acquisition modes and image reconstruction.
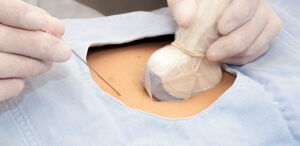
A Sonographer’s Guide to UL Guided MSK Procedures
This in-depth program will provide an overview of the role the sonographer plays in the guided-injection process. It will include discussions of the common injections and injection sites, setting up the procedure room, equipment involved, drawing up medications, preparing the patient, and many more facets of the process.
Latest News
MRI reveals brain changes in people with long COVID
Will Morton - AuntMinnie.com | November 22, 2023
MRI scans have revealed long-lasting microstructural brain changes in patients after COVID-19 infections, according to a study to be presented at RSNA 2023 meeting in Chicago.

Could an Emerging AI System Lead to Earlier Autism Detection with DT-MRI?
Jeff Hall - Diagnosticimaging.com | November 21, 2023
While a recent report issued by the Centers for Disease Control and Prevention (CDC) noted that 30 percent of children with autism were not diagnosed at eight years of age, emerging research suggests that a combination of artificial intelligence (AI) and diffusion tensor magnetic resonance imaging (DT-MRI) facilitates autism detection in children between two to four years of age.
Study Suggests CT-Guided Injections May Restore Sense of Smell in Patients with Long COVID
Jeff Hall - Diagnosticimaging.com | November 20, 2023
One of the more commonly known symptoms of COVID-19 is an altered sense of smell, which may linger for months and possibly years among those with Long COVID. However, an emerging computed tomography (CT)-guided and minimally invasive procedure may provide some relief from this condition referred to as parosmia.
Image Gently®
The Image Gently® Alliance is a coalition of health care organizations dedicated to providing safe, high quality pediatric imaging worldwide. Click the link to learn more.